Have you been diagnosed with diabetes? One of the possible complications is diabetic retinopathy.
You can develop this eye condition if you have diabetes, including type 1, type 2, or gestational diabetes. The longer you have diabetes, the more likely you are to develop the condition.
Keep reading to learn more about diabetic retinopathy and what to expect with the eye condition.
What is Diabetic Retinopathy?
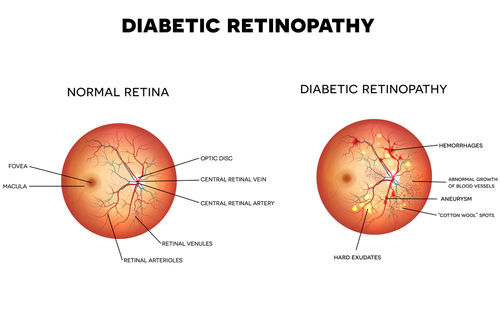
Diabetic retinopathy happens when high blood sugar levels damage the small blood vessels in your retina. The affected blood vessels can close, leading to a blockage that stops blood from passing through.
These blood vessels might swell and leak. But in other cases, new abnormal blood vessels may start to grow on your retina.
All these changes can lead to vision loss. Diabetic retinopathy often occurs in both eyes. Eventually, it causes irreversible blindness without treatment.
Signs of Diabetic Retinopathy
There are usually no early symptoms of diabetic retinopathy. But as the condition worsens, you may notice the following signs:

- Flashes
- Distorted vision
- An increase in the number of floaters you see
- Blurry vision
- Dark spots across your field of vision
- Trouble reading
- Colors appearing faded
- Poor night vision
- Blind spots in your visual field
- Vision loss
Stages of Diabetic Retinopathy
The different stages of diabetic retinopathy are:
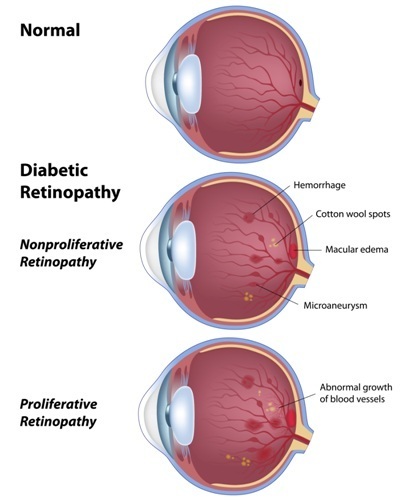
Mild Non-Proliferative Diabetic Retinopathy
The first stage is marked by balloon-like swelling in small areas of the blood vessels in your retina. Rarely does this first stage affect your vision or require treatment.
However, it’s a tell-tale sign that the condition is more likely to progress and decrease your vision. Your eye doctor will advise you to control your blood sugar, blood pressure, and cholesterol at this stage. The more you manage these, the less your risk for vision loss.
Moderate Non-Proliferative Retinopathy
In the second stage of diabetic retinopathy, there’s damage to some of the blood vessels in your retina. Fluid and blood can leak from these damaged vessels and accumulate in the macula.
These fluids leaking causes diabetic macula edema. The macula is found at the center of the retina.
It helps you see straight ahead, vital for reading, driving, and other activities. Reaching the second stage compromises your vision.
Your ophthalmologist may recommend testing your vision every 3 to 6 months to monitor your vision.
Severe Non-Proliferative Diabetic Retinopathy
More blood vessels become blocked with increased leakage of fluid and blood into your retina. As a result, some areas of the retina receive less blood flow and scar tissue forms.
It’s also possible for blood vessels to close off completely. If this occurs, it results in a condition called macular ischemia. Macular ischemia leads to blurry vision and dark spots.
There’s a very high chance of losing sight at this stage. Treatment can prevent further vision loss. However, you’re unlikely to regain the vision you’ve already lost.
Proliferative Diabetic Retinopathy
In this final stage of diabetic retinopathy, it has advanced considerably. New thin and fragile blood vessels begin to grow in your retina and the fluid in your eyes.
These vessels can leak and lead to scar tissue. As the scar tissue becomes smaller, it pulls the retina away from the back of your eye, causing retinal detachment.
Retinal detachment results in the permanent loss of straight-ahead and side vision.
Diabetic Retinopathy Treatment
The goal of treatment is to stop or slow the progression of diabetic retinopathy. Your eye doctor will suggest the best treatment depending on your eye exam results and your specific situation.
Keeping your blood sugar in check is still the most effective treatment for diabetic retinopathy. You significantly minimize the risk of vision loss when your blood sugar is under control.
Other treatment options include:
Anti-VEGF Treatment
Anti-VEGF inhibitors are medicines that minimize swelling of the macula. They also block vascular endothelial growth factor that stimulates the growth of blood vessels.
Blocking the growth factor stops new blood vessels from forming. The treatment is injected into your eyes and accompanied by proper diabetes management. You’ll need repeated injections to maintain the effects of the drug.
Laser Therapy
If diabetic retinopathy advances, the new blood vessels that grow leak fluid and blood in your retina. To prevent this, your eye surgeon can apply a laser treatment called laser photocoagulation.
Laser photocoagulation stops the development of abnormal blood vessels and stabilizes the progression of retinopathy. The light beam used in the treatment is powerful enough to reach the back of the retina so that you won’t need incisions.
Vitrectomy
You may need a vitrectomy if you suffer retinal traction or bleeding. If this occurs, it causes vision loss in advanced diabetic retinopathy.
During the procedure, your surgeon removes parts or all of the blood-filled vitreous and scar tissue affecting your retina. The vitreous is the clear gel that occupies the space between your lens and retina.
Your surgeon will finally replace the vitreous with a saline solution or a bubble of oil or gas to hold the retina in place. You may also undergo laser therapy during vitrectomy to stop further bleeding by removing abnormal vessels causing bleeding.
How to Lower Your Risk of Diabetic Retinopathy
Apart from adequate blood glucose control, you can also do the following to reduce your risk of developing diabetic retinopathy:

- Go for checkups with your doctor
- Keep your blood pressure and cholesterol at healthy levels
- Exercise regularly
- Maintain a healthy diet
- Quit smoking if you’re a smoker
- Get your eyes checked frequently
Prevent Vision Loss from Diabetic Retinopathy
Even if you have 20/20 vision, you can still have diabetic retinopathy. For this reason, our eye doctors at Evergreen Eye Center recommend regular eye exams to diagnose the condition early.

Our experienced ophthalmologists can accurately diagnose diabetic retinopathy and provide timely, best-in-class treatment. Do you have diabetes? Schedule an appointment at Evergreen Eye Center to make your eyes a priority today!

