Diabetic retinopathy is a complication of diabetes that affects the blood vessels in your retina. The retina is the light-sensitive tissue at the back of your eye.
It converts the light that enters your eye into electric signals and sends it to your brain so you can see. If left untreated, diabetic retinopathy can cause permanent vision loss or blindness for people with diabetes. Diabetes is the leading cause of blindness in Americans from the ages of 20-74.
Keep reading to learn about the causes, risk factors, signs, treatment options, and ways to prevent diabetic retinopathy.
What Causes Diabetic Retinopathy?
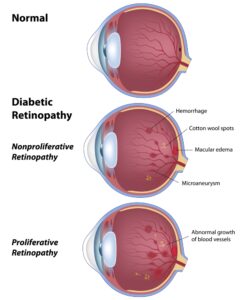
Diabetic retinopathy occurs when high blood sugar due to uncontrolled diabetes destroys tiny blood vessels in the retina. The damaged blood vessels can result in vision loss in the following ways:
- It’s responsible for your sharp, straight-ahead vision, crucial for activities like reading, writing, and driving. The fluid can make your macula swell, causing blurred vision.
- New blood vessels might form on the retina’s surface to replace the damaged ones. But these new, abnormal blood vessels are usually weak. Consequently, they can easily leak blood into your vitreous and block your vision. The vitreous is the clear, gel-like fluid that fills your eye and helps it maintain its round shape.
- The delicate blood vessels in the retina may encourage the growth of scar tissue. The scar tissue can pull the retina away from the wall of the eye, leading to retinal detachment. A detached retina is a medical emergency that can cause severe vision loss or total blindness without prompt treatment.
What are the Signs of Diabetic Retinopathy?
Often, you might not have any signs of diabetic retinopathy in the early stages. However, you may experience the following symptoms as the condition progresses:
- Distorted or blurred vision
- Floaters and flashes of light
- Poor night vision
- Colors looking faded
- Loss of central vision
- Frequent vision changes
- Small dark or empty spots in your vision
- Difficulty reading or seeing distant objects
Risk Factors for Diabetic Retinopathy
Certain factors can increase your risk of having diabetic retinopathy. They include:

- Type 1 or type 2 diabetes
- Poor control of blood glucose levels
- Having diabetes for a long time
- High blood pressure
- Pregnancy
- Smoking
- High cholesterol levels
- Being of Native American, African American, or Hispanic descent
Diabetic Retinopathy Treatment Options
If you have diabetic retinopathy, your treatment options may include the following:
Anti-VEGF Injections
Vascular endothelial growth factor (VEGF) is a protein in the eye that creates abnormal, weak blood vessels that grow in your retina. Anti-VEGF injections block VEGF, delaying the formation of fragile blood vessels in your eye.
Blocking VEGF and delaying the formation of these weaker blood vessels slows or prevents damage from the fragile blood vessels and decreases the threat of vision loss. Repeated anti-VEGF injections have been shown to stabilize or improve vision.
Laser Treatment
During laser treatment, your surgeon will use a laser to seal leaking blood vessels and minimize swelling in the retina. For abnormal blood vessels, the heat from the laser leads to scarring that limits the growth of new, insubstantial blood vessels.
Laser treatment can stabilize your vision and stop it from worsening.
Diabetic Retinopathy Prevention Tips
There’s no way to guarantee you won’t develop diabetic retinopathy if you have diabetes. However, you can reduce your risk of developing the eye condition by following these tips:
Keep Your Diabetes in Check
Well-controlled blood sugar reduces your chances of developing diabetic retinopathy. Ensure your glucose levels are in the recommended target ranges.
If your blood sugar is not under control, work with your primary care physician to develop solutions to get it to a more manageable level.
Watch Your Cholesterol

Get your cholesterol levels tested. If they’re high, your primary care physician can suggest lifestyle changes like weight loss and prescribe medications to treat high cholesterol.
Manage Your Blood Pressure
For people with high blood pressure, taking medications and decreasing stress levels can lower the risk of diabetic retinopathy.

Exercise Regularly
Exercising regularly lowers blood sugar, improves circulation, and keeps your eyes healthy.
Stick to a Healthy Diet
Eating colorful fruits, leafy greens, whole grains, and lean proteins will aid in managing blood pressure, blood sugar, and cholesterol. Following these recommendations can help reduce your risk of developing diabetic retinopathy.
Limit Your Alcohol Intake

Excessive alcohol consumption makes you more likely to develop diabetic retinopathy. If you drink, do it in moderation to minimize your risk.
Dietary guidelines for Americans suggest limiting daily intake to 1 drink or less for women and two drinks or less for men.
Quit Smoking
If you’re a smoker, quitting smoking is in your best interest. The risk of diabetic retinopathy is higher in those who smoke. If you smoke and find quitting challenging, ask your primary care physician to help you.
Schedule Routine Eye Exams
Eye doctors recommend frequent eye examinations for patients with diabetic retinopathy or those at an increased risk of developing the eye condition. With eye exams, your ophthalmologist can diagnose and treat diabetic retinopathy early, which is critical in preserving your vision.
Monitor Your Vision

Pay attention to your eyesight. If you notice sudden flashes of lights, floaters, or black spots in your field of vision, contact your eye doctor immediately.
Protect Your Vision from Diabetic Retinopathy
If you have diabetes and experience any signs of diabetic retinopathy listed above, it’s vital to see the experienced ophthalmologists at Evergreen Eye Center without delay.
Timely diagnosis and treatment can save and preserve your sight. Have you noticed any vision changes, or are you at risk for diabetic retinopathy? Schedule your appointment at Evergreen Eye Center today!

